Architects for East End’s mental health facility say they are creating a “dignified” and “home-like” environment at the nine-cottage, 54-bed home, ensuring “safety and security” for both residents and the surrounding community.
In mid-December, Toronto-based Montgomery Sisam Architects submitted plans to the Ministry of Health for the facility, expected to cost between $10 million and $15 million, on 15 acres in East End, near Health City in High Rock.
The mid-sized firm has designed dozens of similar facilities. Its website lists 102 clients – including the federal and most provincial governments in Canada. Projects include the 10-acre, 192-resident Kipling Acres long-term-care home in Etobicoke, Ontario; the 15-acre Swift Current Long-Term Care Centre in Swift Current, Saskatchewan; and the 55,000-square-foot, three 38-bed inpatient units at St. Joseph’s Hospital for Mental Health Services in Thunder Bay.
The firm told the Cayman Compass it had designed East End’s long-term residential home after confronting community fears that patients could pose a threat to local neighborhoods.
“More often than not,” said Alice Liang, one of seven principals at Montgomery Sisam, “mental healthcare institutions focus primarily on safety and security, assuming that all mentally ill patients will act violently and aggressively.”
However, she said, “evidence-based research has proven that a physical environment that emphasizes surveillance, control that creates a barrier between clinical staff and patients, triggers more agitated behaviors, whereas a therapeutic environment that encourages positive interaction between staff and patients can de-escalate aggression and promote mental well-being for staff and patients.”
Ms. Liang described the specialist design as a “fine balance between … a healing, therapeutic, normalizing environment for recovery and one that ensures safety, security in the most dignified and respectful manner.”
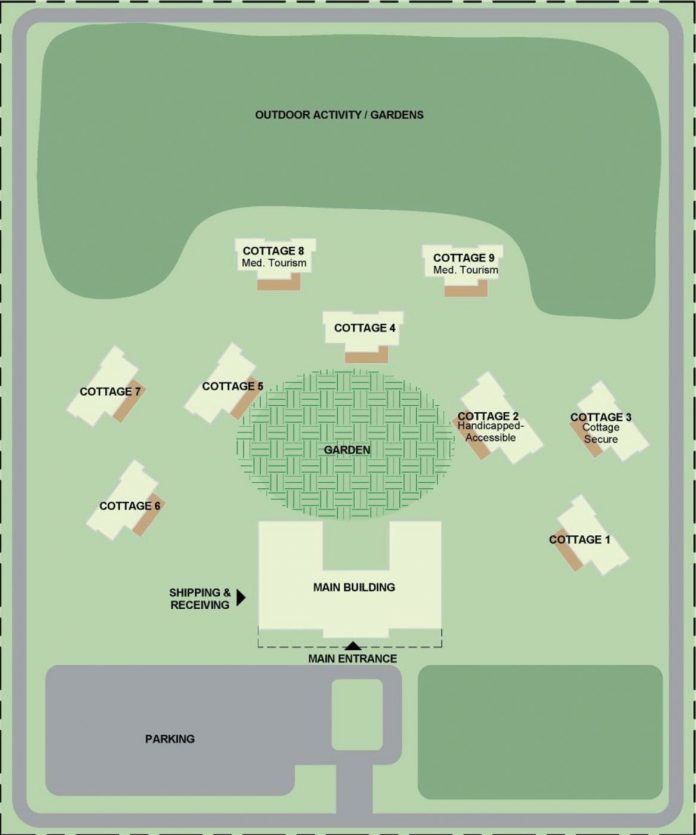
The Ministry of Health’s brief to the architects formally named 54 patients housed in nine cottages, with six people sharing each home, “creating an ideal ‘community’ for residents to gain self-confidence through connecting and socializing with others in the cottage,” Ms. Liang said.
Each patient has his or her own bedroom and washroom, providing “privacy that is fundamental in instilling dignity and self-esteem.” Each cottage boasts a living room, kitchenette and outdoor patios.
“Residents are given agency by having choices and options throughout their daily experience during their stay,” Ms. Liang said.
The cottages “are organized in clusters and embedded within the existing groves of trees on the site to create smaller neighborhoods to further enhance residents’ ability for gradual socialization with larger groups, as they learn to establish broader peer support, promoting a sense of belonging within the community.”
Each design element is calculated to enhance what Montgomery Sisam calls “the vision” for a “therapeutic healing community,” based on similar ideas in the U.S. “where mental health-treatment facilities are situated in rural/pastoral settings to accommodate a range of therapeutic and social activities for residents as they go through their personal journey back to recovery and community integration.”
The Cayman home is roughly based on Gould Farm, a Massachusetts-based residential facility founded in 1913 on 700 acres in Monterey, near Boston. The farm houses 40 “guests” – as patients are called – in three units with 11, 14 and 16 beds. Residents have their own room and share bathrooms and living areas.
Residents are at least 18 years old and, according to Gould Farm’s website, “we help adults with depression, bipolar disorder, schizoaffective disorder, schizophrenia and other challenges begin to rebuild and regain their lives.”
The East End operation will use farmland previously cultivated by Northward Prison inmates. Occupational therapy programs will include gardening, animal husbandry with goats and cows, woodworking, a bakery, cheese-making and a public gift shop.
The program, built around recommendations by longtime advocate for the mentally ill and chairman of the 10-member Mental Health Commission, Dr. Marc Lockhart, encompasses “skills learning and educational programs, encourag[ing] socialization though group activities such as arts and craft-making, music, light agricultural production including tending fruit orchards,” Ms. Liang said.
“In enhancement of residents’ physical well-being, they can engage in recreational sports, leisurely walks and strolls, all in the tranquility of the existing natural surroundings.”
The center of treatment and daily activities is the main building, which she described as “the public face of the facility that is inviting and welcoming for residents, families and visitors,” allowing gatherings in the dining hall alongside group-activity and classrooms.
“The more public spaces, such as the lobby, education/classrooms [will] provide opportunities to welcome and engage visitors from [the] community at large, in participation [at] conferences and other events to further break down any stigma and barrier between the public and those with mental health issues.
“This new facility is definitely not a hospital,” she said, “and it is not an institution. It is to be more residential and ‘home-like,’ a place to heal and recover in a normalized and familiar setting.”
Security — preventing both unauthorized departures and entries – is provided by “biometric analytic detection,” described by Ms. Liang as “an unobtrusive security system around the site perimeter.”
“It will utilize an underground infrared beam and thermo-imaging camera to monitor footfalls that trespass the perimeter.
“Required measures for monitoring and safety alert will be provided invisibly to avoid any intrusive and disrespectful interventions. One such example is the elimination of a continuous high-perimeter fence with new technology of biometric analytic detection buried underground.
“Similarly, the security office for the entire facility is discretely located … providing a strategic vantage point to monitor all movement and activities. One wing of the main building also acts as a designated hurricane shelter,” she said, “where all construction technology and building systems meet … shelter guidelines to ensure residents and staff safety and well-being in case of hurricanes.”
The Ministry of Health will fund and operate the facility, projected to cost $1 million per year. Ministry officials expect construction to begin this summer, and the first intake of residents in mid-2019.
Related Videos