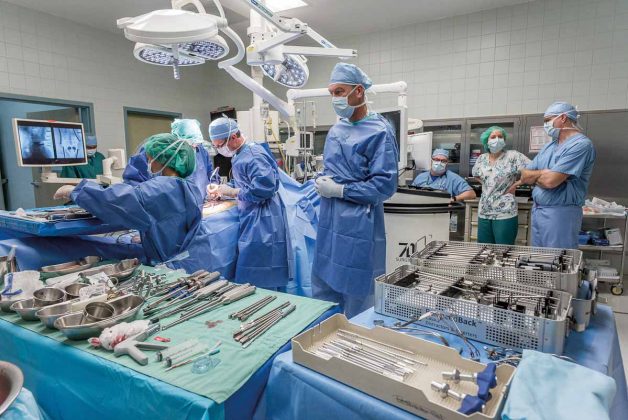
Doctors in the Cayman Islands’ public and private hospitals have responded with a united call-to-arms since the coronavirus reached these shores.
Amidst the global pandemic, in which many overseas healthcare workers have lost their lives while treating COVID-19 patients, they have risen to the occasion with professionalism and large amount of personal bravery.
“This is a war-like situation,” said Dr. Yaron Rado, chairman of the board at Doctors Hospital. “The World Health Organization sent out a call-to-arms and we have responded. This is not a drill; we are the ground soldiers on the frontline. Doctors are dying, nurses are dying. They are risking their lives for the protection of our society.”
But although COVID-19 is a novel, or new, virus, Dr. Rado points out that the strategy of dealing with the disease is not new.
“We are prepared – we have been dealing with infectious diseases for centuries,” he said.
“This is the same way as we would deal with a Middle Ages plague.”
Along with the other healthcare facilities on-island, Dr. Rado and his colleagues knew the virus would eventually reach Cayman, and all quickly mobilised to deal with the impact.
Doctors Hospital is providing drive-through testing with results provided in as little as four hours and remains open for other healthcare needs, including acute and chronic conditions, with the operating room in use for urgent clinically indicated surgery.
The facility is also working with HSA to ease the public hospital network’s patient load.
“In particular, our new cardiac services have meant that we are in a great position to treat urgent cardiac cases in a timely, efficient manner,” said Dr. Rado.
The hospital’s maternity unit has also welcomed an average of five babies per week into the world during the pandemic.

HSA prepared
Dr. Elizabeth McLaughlin of the HSA agrees that the islands were well-prepared for COVID-19.
“We have been preparing for public health emergencies over the years,” she said.
By early March the HSA had arranged to acquire off-site facilities to house patients should the need arise, forged tentative agreements with private physicians in case additional clinical staff were required, and invested significant funds into personal protective equipment and ventilators.
The HSA can treat up to 30 COVID-19 patients in Grand Cayman and six in Cayman Brac, with capacity to care for 16 ventilated patients and more if necessary.
But while they are trained and equipped to deal with the coronavirus crisis, there are still a number of new personal practices that each healthcare worker has had to adopt.
Dr. McLaughlin, who is the clinical head of Accident & Emergency and EMS, said that continually wearing a mask while working is one of the more simple but challenging adjustments for her, personally.
“I know this may be an unexpected response, with all the information of persons dying, and lack of ventilators,” she said. “Presently, here, we have adequate ventilators and can meet the current demands but working behind a mask, and managing persons behind a mask, can have an impersonal feel to it. It does take some adjusting to ensure effective communication.”
She also said that the humanity of healthcare workers often becomes lost in the process of dealing with the coronavirus and treating all of the other known and regular health issues in an era where all patients must be presumed as COVID-positive.
“The risk is there,” she said. “The news reports are a constant reminder…
I am also fortunate to be surrounded by colleagues and teams who are hardworking and compassionate, and my concern is for them. They inspire me to stay focused, to be creative and strive for the best care for our patients.”
The HSA is part of the National COVID-19 Response Task Force alongside Doctors Hospital, Health City Cayman Islands and The Cayman Islands Medical and Dental Society.
The HSA has also been working with a number of volunteers from Cayman Islands Red Cross. who are assisting with the coordination of COVID-19 screening at onsite and drive-through screening tents.

Health City scare
Health City Cayman Islands has had its own share of scares, with four staff testing positive for the virus after a cruise ship passenger died from COVID-19 at the hospital in March. All four members of staff have now recovered.
Health City, however, was closed for two weeks for emergency and non-emergency admissions while strict new infection-control measures were implemented.
“As a frontline healthcare professional working in emergency and intensive care, there is a lot of apprehension, coupled with fear of getting infected while dealing with COVID-19 patients,” said Dr. Mahantesh Patil. “So far, from the world experience, frontline healthcare professionals are at increased risk of getting COVID-19 and some unfortunately did succumb to COVID-19.
“(This is) more so in the emergency and ICU area, as the therapy gets intense with multi-organ support needing the constant support of intensive care nurses and doctors.”
Some of the Health City staff went through the H1N1 pandemic in 2009, which has helped them cope with the current crisis.
“What drives us in these difficult times is the utter sense of duty and commitment to our patients over our personal interests,” said Dr. Patil.
Health City has earmarked 47 beds for patients affected by the virus, including 11 ICU beds with ventilatory capacity.
The healthcare facility is also rolling out an emerging treatment for COVID-19 using the plasma of patients who have previously been infected and who now have antibodies to the virus. Health City is awaiting final approval for the treatment, which has already been endorsed by the National COVID Task Force.
The facility also offers sophisticated treatments like Extra Corporeal Membrane Oxygenation for patients in advanced respiratory failure who are not responding to standard ventilation, adding to the country’s capacity to fight the deadly pandemic.
Related Videos