More than 20,000 people – almost a third of the islands’ population – have now been tested for the coronavirus.
But the diagnostic tests – involving chemical analysis of a DNA sample collected from a nasal swab – can only tell us so much.
A new wave of ‘antibody testing’, which began in the last week, will help provide public health officials with more information about the prevalence of the virus throughout the islands.
Back in May, Cayman Compass journalist James Whittaker got the COVID-19 swab as part of a feature story explaining the testing process. On Tuesday, in a sequel to that story, he visited Health City Cayman Islands to do the same for the new antibody tests.
There will be blood
First, they probed my nose; this time, they want my blood.
Two months after taking the COVID-19 diagnostic test, I find myself back in the role of journalistic guinea pig, stretching out my forearm to offer a plump green vein for the new antibody test.
The first test told me I did not have the coronavirus – at least not at that time. This one will tell me if I have ever had COVID-19 and if I potentially could have any immunity to the virus.
It starts with the unpleasant, but familiar, experience of giving a blood sample. You know the drill here.
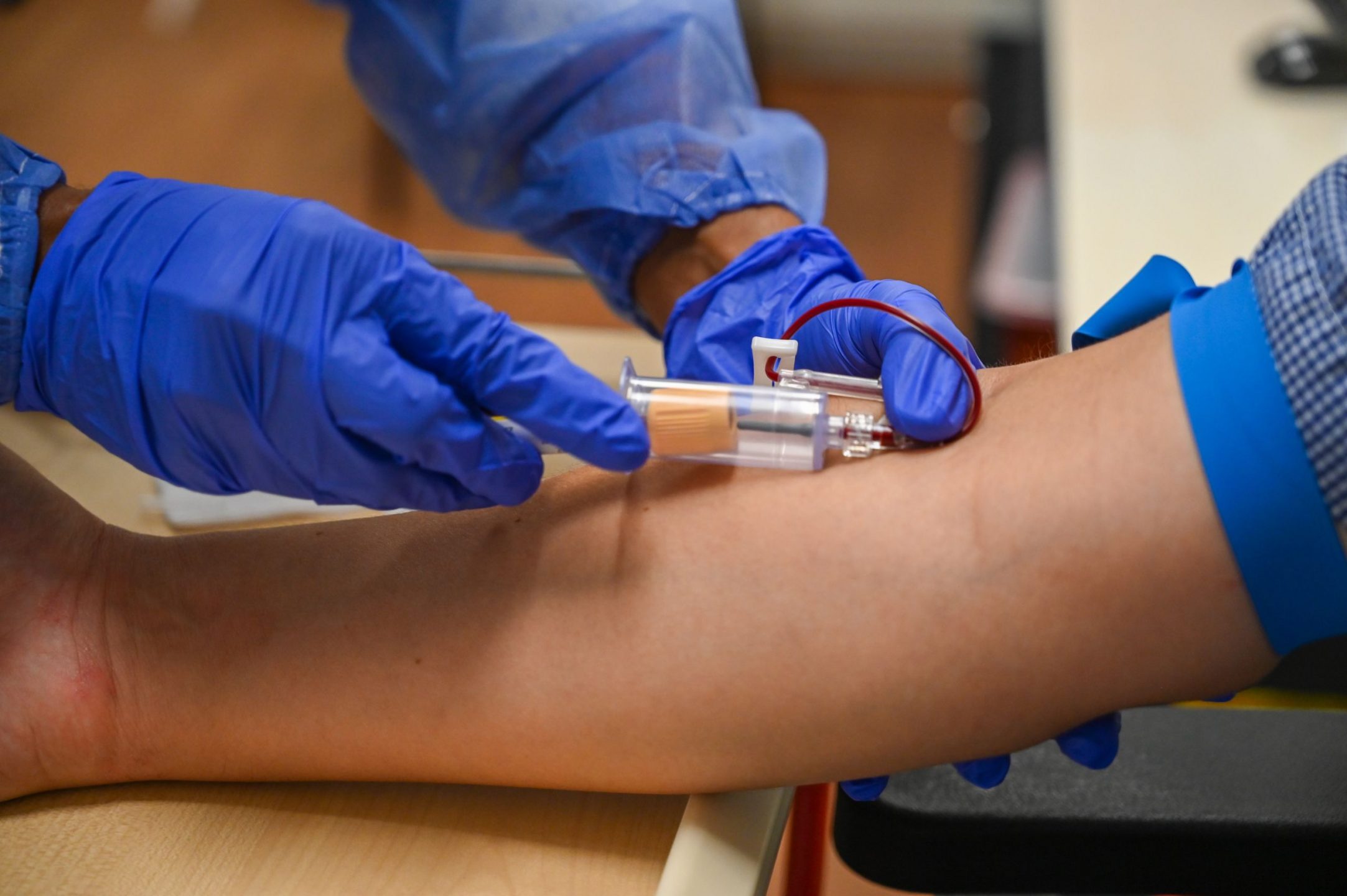
The nurse tourniquets my arm, inserts the needle, and the tube fills with dark red fluid.
The sample is dispatched into a cooler, ready to be conveyed to the lab.
Two tests: What’s the difference?
While the sample is being processed, I sit down with the hospital’s medical director, Dr. Dhruva Kumar Krishnan, and ask him to explain in simple terms what the difference is between the two types of tests.
“The PCR test, as you know, is a nucleic acid amplification test or a polymerase chain reaction…” he begins.
It is clear he has grossly overestimated me.
He reads the facial cues and continues.
“In lay terms, it is a swab which is taken from your nasal cavity and if that comes back positive, that means you have COVID-19.”
This is more like it.

Basically, the first test tells you if you have the virus at that moment. It typically comes up positive within 5 to 14 days after you contract the virus.
That is invaluable from a diagnostic perspective. That’s how healthcare providers know if a sick patient has the coronavirus and helps them decide on treatment options.
From a data perspective, however, there are limitations.
More than 20,000 people have been tested in the Cayman Islands so far, with only 196 confirmed cases, as of Thursday.
So, does that mean that less than 1% of those tested has had the virus? No. It means that less than 1% had the virus at the time they were tested.
While that is a useful indicator that the prevalence of COVID-19 in the Cayman Islands is relatively low, it is far from the whole story.
Cayman has had an extraordinarily high number of incidences where people have been found to have the virus despite not showing any of the symptoms, such as fever, dry cough, and loss of taste or smell.
If those asymptomatic cases had not been picked up during screening tests of frontline workers, those people and the country’s public health officials would never have known about them.
It is likely, therefore, that many others have had the virus without even being aware. How many, and am I one of them? That is where the antibody tests come in.
Antibodies: A natural defence system
Antibodies are proteins produced by your immune system in reaction to an invading organism, such as a virus.
They are part of your body’s natural defence system against disease.
High-tech testing equipment, such as the Roche analyser machine which will process my sample, can detect antibodies specific to the coronavirus.
If they are present, it will signal that I have had the virus at some point.
It may also mean I have developed a degree of immunity to COVID-19, but the jury is still out on the extent to which this would protect me from future infection.
The test doesn’t differentiate between past and present infection, so it will not be clear from the result whether I currently have the virus or if I had it several months ago.
What the test will definitively determine is if I have had exposure to COVID-19.
Along with the Health Services Authority, medics at Health City are carrying out daily antibody tests to help determine what proportion of the country has been exposed to the coronavirus.
At a recent government press conference, Chief Medical Officer Dr. John Lee estimated that as much as 15% of the population could have had the virus.
How the test works
As Dr. Krishnan and I converse, my blood sample is being placed into a centrifuge to separate the liquid portion of the blood, known as plasma, which contains the antibodies.

The sample is then run through a Roche Cobas E411 analyser machine. This is a piece of equipment that Health City had in its lab anyway and is used to test for antibodies in various viruses.
What is new is the ability of this machine to test for the coronavirus.
I had already asked Krishnan for a simple explanation of how it does this. His answer: “Quantitative electrochemiluminescence.”
Some processes are not so easy to put in lay terms. The best we can say is that there is a chemical process that takes place and if the antibodies are present, they will light up.
“You will get an email,” Krishnan assures me.
Two types of antibodies
The Roche Analyser test, approved by Public Health England, has been proven to be 100% accurate. But it also has its limitations.
While it will show if I have virus-fighting antibodies or not, it won’t show which type. And the distinction is crucial.
Immunoglobulin M, or IgM, is the initial antibody produced in the active phase of the virus.
If IgM is present in the plasma, then that would likely mean I have a current case of COVID-19.
Immunoglobulin G, or IgG, is the antibody that develops later and stays in the system longer, providing a degree of immunity against future infection.
If I have IgG proteins, then that is good news – a potential shield against future infection.
As I wait for the test results, it is hard to know what to wish for.
A positive result might mean I have the ‘golden ticket’ of immunity and can worry a little less about contracting a serious case of COVID-19.
On the other hand, it might mean I have the virus now and am about to get quite sick.

In the future, Krishnan says, test kits may be developed that can differentiate between the two. For now, he believes the best policy is to use this type of testing to supplement the PCR test – the nasal swab I had a couple of months ago.
In combination, the two results can determine if a patient has a current or past infection.
A cough in February
Personally, I am unsure if I might have had the virus or not. I had a cough in February that lingered into March and, amid the constant news reports, I wondered if it might be an after-effect of COVID-19.
A lot of people are in a similar position, says Krishnan.
He has seen several patients who he believes may have had the virus earlier in the year – before it was really on the radar in Cayman or there was capacity to test for it.
“All of them had some history of travel and a chronic cough or flu-like illness, at least one or two were admitted to hospital, but we never suspected or thought of COVID at that time.”
To some extent, these antibody tests will determine if those who swear they had COVID-19 in January were right.
The results won’t specify when a patient had the virus, but combined with anecdotal evidence, they will help determine when it first arrived in Cayman.
Krishnan believes the islands’ tourism industry and the extent to which COVID-19 hit cruise ships, in particular, suggests the virus was slowly and quietly moving through the community long before it was first identified.
“We got into the lockdown mode very early. After 15 days, we should not have seen any new cases, but there were still cases cropping up, so there was some amount of community transmission going on asymptomatically.
“It probably was on our shores before we even realised.”
Double-negative
If there was a number of Cayman Islands residents that did contract the virus earlier this year, I can now definitively say I am not one of them.
My results arrive, as promised, via email the same afternoon.

The report states, “NON REACTIVE-Negative for anti-SARS-CoV-2 antibodies.”
For me, that means I must remain vigilant. I am still at risk of contracting the virus.
For public health officials, it is an extra data point to help them calculate the extent of the islands’ exposure to this virus.
Related Videos