Over the next few weeks, thousands of Cayman Islands residents will be tested for the coronavirus. In an effort to demystify the process and set his own mind at ease about a lingering cough, Cayman Compass journalist James Whittaker got swabbed for COVID-19. In a special feature, we follow the progress of his sample, from its uncomfortable extraction to the moment the results arrive in his email inbox. In between times, the scientists, doctors and lab techs talk us through the sophisticated process of determining who has the virus and who doesn’t.
Part 1 – The Swab
I had seen the videos. People screaming, sneezing or collapsing in fits of laughter as the swab probed uncomfortably far up the nasal cavity.
“It was like being stabbed in the brain,” according to one social media account I probably shouldn’t have read.
I was prepared for an experience that would be at best uncomfortable and at worst akin to a pre-frontal lobotomy.
Booking a slot, at least, was relatively painless. I put in a call to the CTMH Doctors Hospital Care Centre on Friday and by 10am Monday I was rolling up to the drive-through testing lane.
I came to a stop in front of a barricade beyond which a trio of medics waited in the shade of a tented canopy.

After what seemed like an improbably swift set of introductions through the car window, the notorious swab was being withdrawn from its sterile scabbard.
It resembled an elongated lollipop stick. The kind you tell kids not to put up their noses.
“Lean back and take a few deep breaths,” the nurse, Kadian Atkinson, advised – perhaps detecting a hint of cowardice.
With the procedure being captured on video, it was important, for the sake of self-respect, if not for viewer entertainment, that I stayed cool.
I gripped the steering wheel, perhaps a little tighter than was necessary, and tried not to watch as the surgically gloved hand advanced towards my right nostril.
It tickled just a little at first and I was tempted to sneeze. Still, it was difficult to see what all the fuss was about.
But the swab just kept on going, journeying beyond the point where the distinction between nose and whatever lies beyond was particularly clear.
I opened my eyes for a second and wondered if Nurse Atkinson was smiling. Was there, perhaps, a sadistic pleasure to be had in watching me squirm? Behind the surgical mask and motorcycle-style visor, it was hard to tell.
Just as the urge to laugh or sneeze or squeal began to feel uncontrollable, the pressure eased and the swab began its retreat.
I breathed out one more time and it was done. The nurse dispatched the sample into a test tube, filled with a chemical solution that would immediately inactivate the virus, if it were present.
That five-second journey from nose to test tube is perhaps the most dangerous for the medics involved.
Now that she was no longer probing the deepest recesses of my nasal cavity, I was clear-eyed enough to see Nurse Atkinson and her colleague, nurse Jasmine Minott, in their proper light – committed professionals putting themselves in harm’s way to keep the community safe.
For most of us, encountering someone with coronavirus is something we are taking exceptional measures to avoid. For these guys, it is an occupational necessity.
My part in the process was over and it had taken less than 10 minutes from start to finish. I have waited longer for a cheeseburger.

Critically, I hadn’t made a fool of myself on a national broadcast. The more important test was yet to come: Did I have the coronavirus or just a mild case of man-flu?
Part 2: The lab techs get to work
My role may have been over, but my DNA sample was just beginning its journey.
Things were about to get complicated.
The test tube, labelled with a barcode linking to the identification information diligently triple-checked by clinical analyst Rico Ponton at the drive-through, was placed in cold storage with the rest of the day’s samples.
That’s a fancy way of saying they put it in a cooler.
Within half an hour, two gowned and masked medics arrived to collect the morning’s samples. It’s a short walk to the sterile facility that has been converted, in a matter of weeks, into a molecular laboratory capable of testing for COVID-19.
On a thick glass sliding door inside the lab, a printed sign warns ‘Stop – Bio-Hazardous and Infectious Materials’.
On the other side of the glass is lab manager Gayon Allen-Goulbourne.
This is where the magic happens or, as I am quickly corrected, this is where the science happens.
It is her job to take the sample and extract a workable specimen containing human DNA and, if it is present, the RNA that carries the signature code of the coronavirus.
Allen-Goulbourne’s life has changed dramatically in the past six weeks.
Her skills as a laboratory technician have propelled her into the middle of a global health crisis. The work that she along with her counterparts at the Health Services Authority do in these labs will help determine the prevalence of the virus throughout the country and dictate if and when the economy can reopen.
It is a tremendous responsibility and one she takes great pride in shouldering.
She gets emotional when she talks about her 3-year-old and her 1-year-old at home and how her husband Hilzan is caring for them while juggling his own work as an IT consultant.
But when there is a job to be done, she is 100% focussed.
The swab arrives in her lab in a test tube, bathed in solution – the virus-inactivating chemical that has made it safe to handle.
Using a pipette, she extracts the liquid and transfers it to another plastic tube, with a special filter attached.
My sample slots along with 23 others, all carefully labelled and placed into a centrifuge.
The spinning process removes the liquids, leaving a workable sample of DNA and RNA – the two types of nucleic acid found in human and viral cells.
Now it is ready to be tested.
Part 3: Analysing the sample
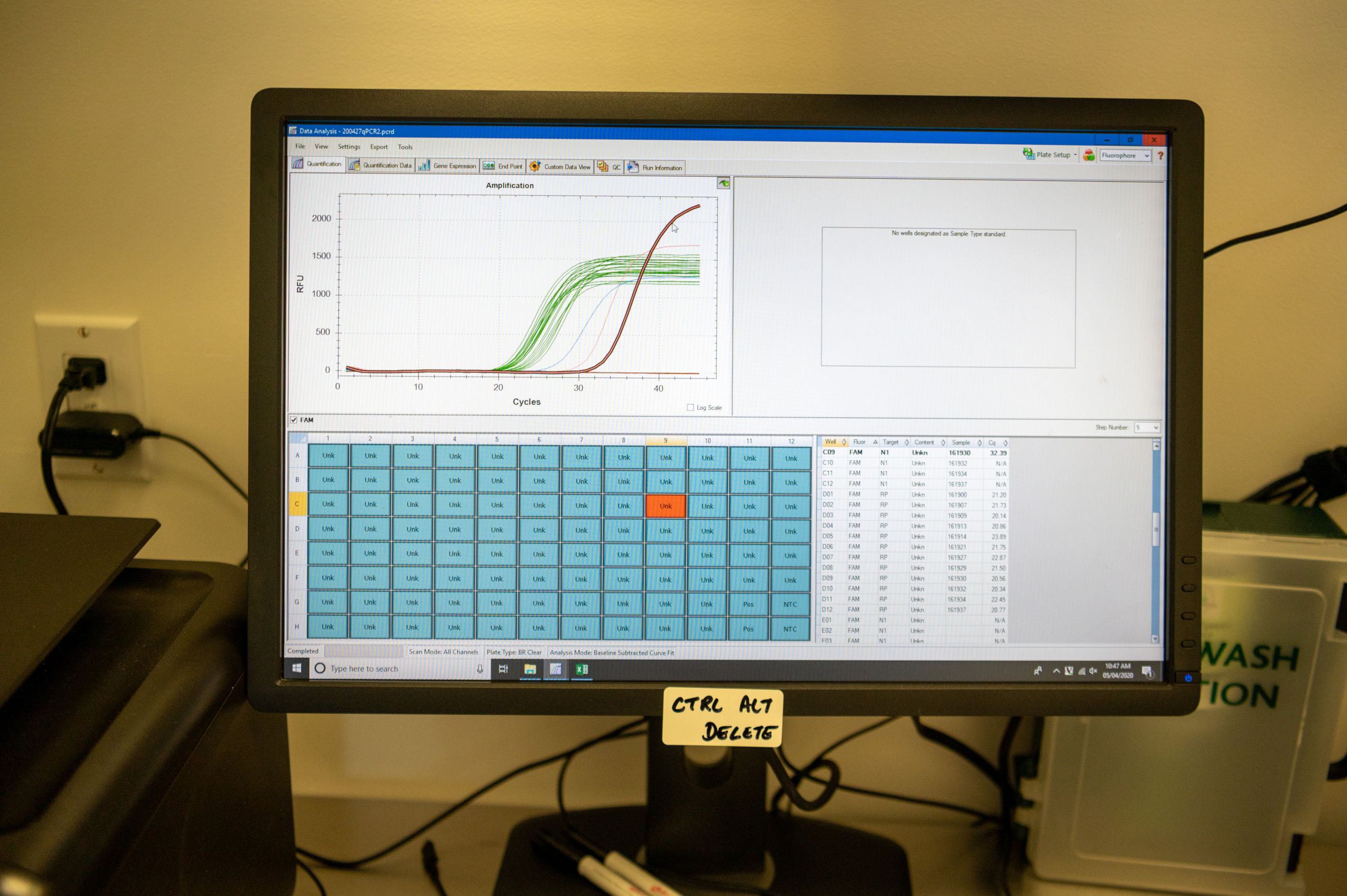
Some time later, on the other side of the sliding glass door, green and blue lines spiral across an evolving digital graph on a computer monitor.
“No red. That’s good,” explains Dr. Frank Koentgen as he watches the lines slowly curve upwards.
The green lines correspond to human DNA. Blue is for the coronavirus control samples, pre-loaded into the test. Red would indicate the presence of the virus in one of the samples currently being run through a Polymerase Chain Reaction machine.
The machine, despite the critical role it plays in the fight against a global pandemic, is not especially impressive to look at. It is a small boxy contraption, the uniform beige of an office printer.
The comparison is apt because it is basically a molecular photocopier. Its core job is to amplify DNA strands, present in the samples, to the point where they show up on Koentgen’s graph.

Along with the genetic samples, substances that cause chain reactions have been loaded into the machine.
“Those are the chemicals and enzymes that multiply the DNA samples and the RNA of the virus (which is converted to DNA in the same process) if it is present, and illuminate it,” Koentgen explained.
For now, the signs are good. But on its current setting, it is a 90-minute process and there is still plenty of time for the COVID-seeking fluorescent probes to hit their mark.
By way of demonstration, he produces a print-out of a positive result. A thick line, the pinkish-red of watery blood, spikes through the gentle green parabolas that dominate the graph.
“If we see red, we know we have COVID,” he says.
Part 4: The backstory
The fact that Koentgen is here at all, watching the genetic code from the back of my nose expressed as coloured lines on a graph, is a small miracle in itself.
An entrepreneur and renowned biotech scientist, he made his name as the co-founder of Ozgene, an Australian company that produces genetically modified mice for drug validation and medical research trials.
Some time ago, Koentgen, who is a dual German and Australian citizen, established a new company in Cayman’s Enterprise City, focussing on global research services.
He met Dr. Yaron Rado, the chairman of Doctors Hospital, over a glass of wine – a commonplace encounter in a small place like Cayman, before the coronavirus made such pleasantries impossible.
As fellow Germans in the medical field, they found they had much in common.
Just a week before Cayman’s first coronavirus case, Rado was readying the hospital for an anticipated outbreak.
“I got a WhatsApp from Frank saying I am coming from Perth on Friday, should I bring a COVID tester?” Rado told me in an interview immediately after I had been swabbed.
He added, “I didn’t know at the time what this entailed, but I knew that testing was going to be the determining factor in how the country came through this, so I said, ‘Sure, let’s do it.’”
Watching cars slowly roll up to the medical tent, Rado reflected that the process looks smooth and simple.
Patients (though that is not exactly the right word as the vast majority are essential workers getting screening tests) roll up, flash their ID, squirm for a moment as they get swabbed, then drive away. A few minutes pass and the next car arrives, and the process repeats itself.
Establishing that system was a huge logistical challenge.

Rado credits Joanne Deys, president of Ozgene LLC USA, who arrived with Koentgen to help set up the lab, as the brains behind the operation.
“It is like an industrial machine line. We had to look at the whole process from data entry in the care centre to the automatic email you are going to get with your result.”
Part 5: The waiting game
It is the few hours between swab and email that is perhaps the most tense for those of us who have passed through the drive-through.
Most will find out they don’t have the virus and they can breathe a little easier as they go about their daily lives.
An unfortunate few, including some with mild or no symptoms, will be told they do have COVID-19 and they must go into isolation.
With that will come the awkward process of retracing every step, confessing to any breaches of the regulations as they assist public health teams in tracing every interaction over the past days and weeks.
There will be inevitable trepidation over the possible onset of symptoms or, perhaps worse, the guilty premonition that you may have passed on the virus to someone less able to withstand its effects.
I felt a pre-sentiment of those emotions as I left Koentgen waiting for the final read-out from his PCR machine.
Faces from the past few weeks passed through my mind – the elderly lady who stopped to pet my dog, the overweight man who squeezed past me in the supermarket, the pedestrians and joggers I passed as I huffed out deep breaths of exertion on a rare morning bike ride.
If I did have COVID-19, any of them might have it, too.
Part 6: The result
Thankfully, I didn’t have to wonder for too long.
I had been home for just a few minutes, preparing to watch the government’s daily press conference, when an email pinged in my inbox with a pdf attachment declaring me officially negative for COVID-19.
Around an hour or so later, I was jotting down notes from the briefing, when Dr. John Lee announced an addition to the numbers he had given earlier – a batch of 24 new results, all negative – had come in from Doctors Hospital.
It had taken a little over five hours from swab to being an official statistic on national television.
In truth, I never really expected I had the coronavirus, but it was a relief to know for sure. As thousands of Cayman’s residents go through the process over the next few weeks, I wish them the same good fortune in the hope that we can come through this crisis, and something close to life as we knew it can resume.
Related: Frontline workers urged to take COVID tests
Related Videos






Where’s part VII? Disposal of samples. Why the most important part is always overlooked? Steps taken to dispose hazardous material?? With photos of course and names.
Perhaps the singularly most helpful, informative and uplifting article on the epidemic to date. Thank you James and the Compass for your thoughtful coverage of this crucial aspect of our fight against this pernicious disease. High fives to Drs Rayo and Koentgen for their foresight in bringing it here early in the battle. It’s a real ray of hope to think that we may now have the potential to find and isolate every case on the island over time… if we just continue to maintain our distance until testing can do its job.