By: Michael Klein and James Whittaker
Once the borders reopen to vaccinated travellers, Cayman Islands leaders are anticipating that some degree of exposure to COVID-19 is inevitable.
Governments across the world have accepted that communities must live with COVID, using vaccines and a variety of other control measures to keep the threat from the virus manageable.
But what exactly is the risk from COVID at this point?
Using data from the UK, US and comparable island communities like the British Virgin Islands and Bermuda, Compass journalists Michael Klein and James Whittaker examine what the numbers say about some of the key areas of concern for Cayman.
How many people could be infected with COVID-19 if the borders reopen?
Once vaccinated tourists are allowed to enter the Cayman Islands without quarantining, it is inevitable that COVID-19 will be back in the community. The re-emergence of community transmission suggests it may already be back, though it is possible that, at this stage, this outbreak may be contained.
Although the border reopening has been pushed back to 2022, Premier Wayne Panton has acknowledged that can’t be a permanent measure and ultimately the virus will be back and “we will have to learn to live with it and manage it”.
Vaccinated people can carry and spread COVID, albeit not at the same rate as those who have not been immunised.
If COVID-19 takes hold in Cayman and the exposure to the virus reaches the levels now seen in the UK, which has lifted all restrictions on movement and gatherings, we could expect a high number of people to contract the coronavirus.
The UK is currently seeing about 38,000 cases each day. The equivalent daily rate, adjusted for Cayman’s population, would be 39 positive cases per day.
At the worst of the crisis in the UK – before a majority of the population had been vaccinated – the rate was much higher, equivalent to 85 cases a day when adjusted for Cayman’s population size.
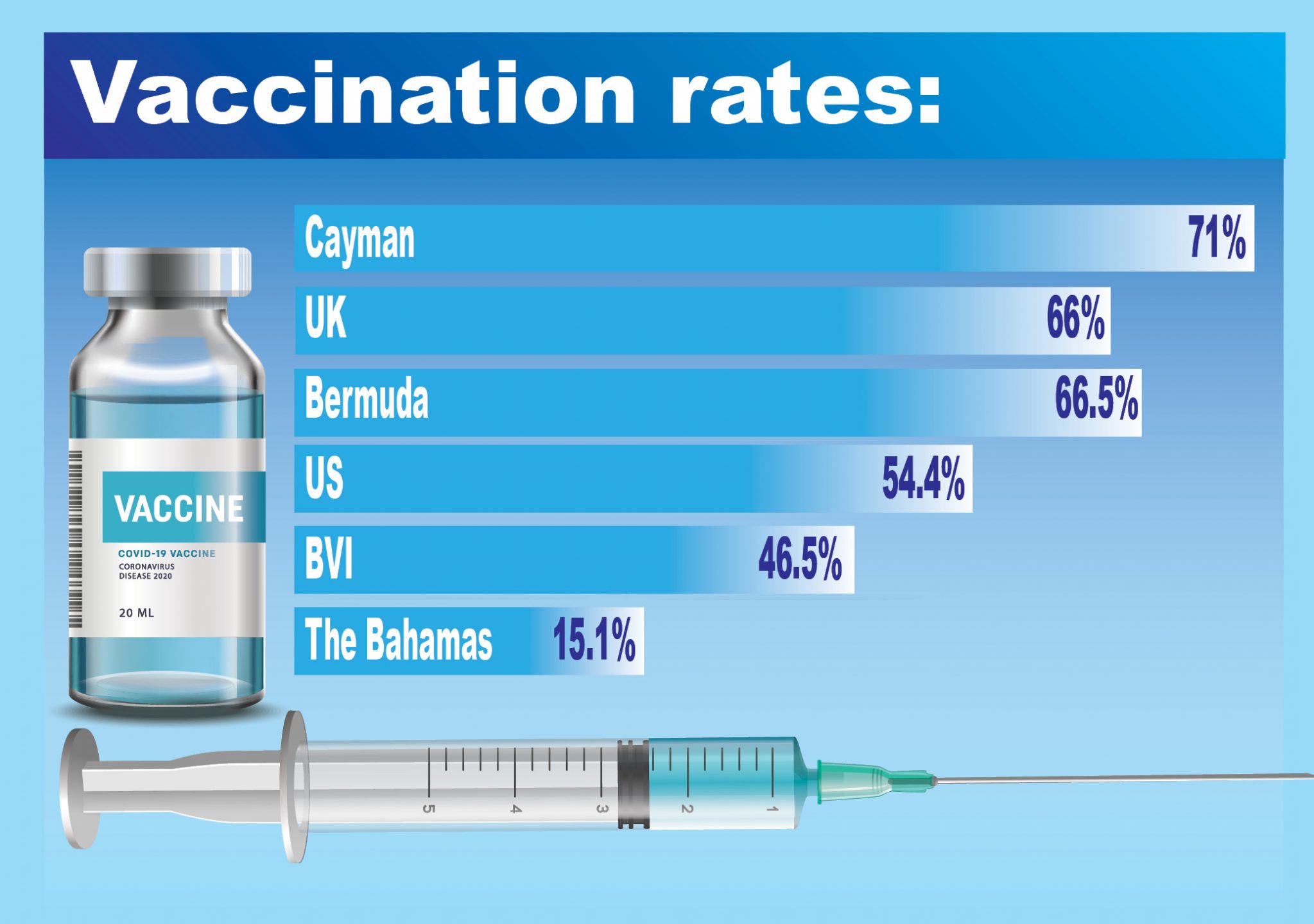
If we look at a small island population like Bermuda, potentially a more relevant comparison in terms of size than the UK, the infection rate hit 79 cases per day during a deadly second wave in April and averaged more than 80 per day during a current major outbreak. Active COVID cases have since reached a record 1,083 in Bermuda.
The BVI, which saw a significant COVID surge in July peaking at almost 1,600 positive cases, is down to 50 active cases. It is worth noting, however, that the BVI’s vaccination rate of 46.9% is much lower than in Cayman, although it jumped after the surge that resulted in 35 deaths in the islands.
As a result of COVID outbreaks, the total cases in Bermuda (4,072) are five times higher than in Cayman (758).
So far, in Cayman more than 52,000 tests carried out on frontline workers and travellers to and from Cayman, on average returned 0.53% positive tests this year. The highest daily number was 3% positive tests, when 24 positive cases were detected on 6 Sept.
How many people would need hospital treatment?
The number of positive cases Cayman can expect to see each day is relevant, especially to determine when additional mask mandates and other measures are necessary. But the number of hospitalisations is much more crucial.
While the potential for 40 or more cases per day sounds dramatic, 18 months of COVID data tells us that the fraction of those that will become seriously ill is relatively small.
At the height of the crisis in the UK, before anyone was vaccinated, hospitals were treating nearly 40,000 patients each day, equivalent to 40 a day in Cayman.
Today, the UK, which has a slightly lower vaccination rate than Cayman, is seeing far fewer hospital cases – around 8,000 a day. Adjusted for Cayman’s population size, that equates to eight people needing treatment in hospital on a given day.
The Bahamas has seen 400 hospitalisations and 19 deaths from COVID in the five weeks from 1 Aug. More than 95% of the hospitalisations and deaths affected unvaccinated people. Only three partially vaccinated people required hospital treatment and no one who was vaccinated died.
Importantly, only 15.1% of Bahamians are currently vaccinated.
The peak number of hospitalisations in Bermuda was 45 in July. Bermuda is currently experiencing another outbreak with 42 people in hospital and 11 of those being treated in intensive care. This is almost triple the number from the week before. Bermuda has a vaccination rate of 66.5%, slightly below Cayman’s at 71%.
These are the kinds of figures that would be the potential worst case if COVID sweeps through the islands. Limiting entry to vaccinated travellers only, who also have to present a negative test before getting on the plane, is likely to lower infection rates and ensure that figure is smaller.
At the beginning of the pandemic, governments around the world were most concerned that the coronavirus could overwhelm healthcare systems. A year-and-a-half later, they had time to prepare and address the most serious shortcomings.
Health Minister Sabrina Turner reiterated last week that Cayman’s healthcare services are prepared to deal with a wider COVID outbreak.

She said she has no doubt that government and private sector healthcare providers will be able to respond “when and if the virus enters our community”.
Turner added, “Our local healthcare infrastructure has been strengthened throughout the past 18 months to ensure that facilities and programmes are ready for any potential surge in the virus.”
The expanded capacity of beds and ventilators includes seven ventilated beds at Cayman Islands Hospital and in-house capacity for a further 20 beds and ventilators in the surgical unit, and an additional six beds in the respiratory care unit. More bed capacity would also be provided by Doctors Hospital and Health City Cayman Islands.
How many people could need to be on a ventilator?
Not all COVID hospital cases require urgent or intensive care. Critical shortages at the start of the pandemic concerned ventilators and masks. This is no longer the case.
In the UK, there are currently 1,450 COVID-19 patients on ventilators, a figure that would equate to 1.5 people in Cayman. Before the UK began vaccinating the adult population, the peak was just over 4,000, equivalent to 4.3 people in Cayman.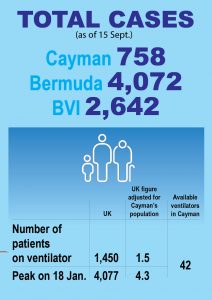
In total, there are 42 ventilators on island – 20 at Cayman Islands Hospital and another 22 at Health City – enough to deal with even a worst-case scenario.
How many people could die?
If we look at the entire duration of the pandemic in the UK, just over 7 million people have contracted COVID and almost 135,000 have died.
Based on those figures, if Cayman had been open to travel and our population had experienced the same level of exposure as the UK, as many as 140 people could have died.
Bermuda, which has the same size population as Cayman and has had limited restrictions on travel, has seen 42 deaths. The BVI with half of Cayman’s population size has suffered 37 deaths.
However, those figures ignore the impact of vaccinations.
If we look at the deaths in the UK since 1 May, when the vaccination programme started to have an impact, the numbers are lower. There have been about 6,000 deaths since that time, equivalent to 6.3 in Cayman or a rate of 18 per year, if adjusted for Cayman’s population size.
Again, this number is predicated on a full-scale outbreak occurring in Cayman and the virus taking hold to the same extent it has in the UK.
In small island territories like Bermuda and the BVI, the number of COVID deaths was proportionally lower than in the UK and, for the most part, the result of sporadic large-scale outbreaks.

Still, it is impossible to statistically rule out deaths from the coronavirus, once Cayman fully reopens its borders, even if Cayman’s high vaccination rate increases and larger outbreaks are prevented.
For context, there were 215 deaths in Cayman last year from all causes.
Importantly for Cayman, the experiences in other countries confirm that the vast majority of hospitalisations and almost all deaths will affect unvaccinated adults.
What is the difference in risk for those who are vaccinated versus those who are unvaccinated?
All available data reinforces the importance of vaccinations.
As of the second week of September in Bermuda, 133 people had been admitted to hospital with COVID-19, 22 of whom subsequently died, since the vaccination programme began in the territory on 11 Jan.

Five of the hospital admissions were fully vaccinated, 12 were partially vaccinated and 116 were not vaccinated. None of the patients who have died in Bermuda were fully vaccinated.
This is consistent with data reported in the US.
Across all US states, the number hospitalisations of unvaccinated people was 48 times higher and the number of deaths from COVID-19 was 21 times higher than for people who were vaccinated.
A study released by the US Centers for Disease Control and Prevention on 10 Sept. found that the unvaccinated are 11 times more likely to die and 10 times more likely to be hospitalised. Keeping hospitalisations low is particularly important given that some studies have put the mortality rates among coronavirus patients in hospitals as high as 27%. In Bermuda, that rate was 16.5% in the first eight months of 2021.
If Cayman were to experience a COVID outbreak on the scale seen in the US, then the data suggests that, in the worst case, two people could potentially die from COVID-19 despite being vaccinated.
What is the risk to get infected when vaccinated vs unvaccinated?
The vaccines are designed to stop serious disease, hospitalisation and death, and they are doing that very effectively – even against the Delta variant.
Although breakthrough cases are expected and have received a lot of media attention, it is important to bear in mind that breakthrough infections are still uncommon, and breakthrough disease is rare.
The latest study cited by the CDC indicated that unvaccinated people are on average five times more likely to get infected. This has varied over time as the Delta variant took hold in the US.
Data released by the CDC has also shown that vaccinated people infected with the Delta variant can carry detectable viral loads similar to those of people who are unvaccinated, though in the vaccinated, these levels decline rapidly.
That suggests a fully vaccinated person who experiences a breakthrough infection can spread the virus just as much as an unvaccinated person but for a much shorter amount of time.

Generally, it is also expected that symptomatic breakthroughs are more contagious than asymptomatic breakthroughs.
In the UK, a study between December 2020 and July 2021 found breakthrough infections affect 0.02%, or one in 500, of vaccinated people. For partially vaccinated people the rate was 0.05%.
The study, based on self-reported patient data, found that people who contracted the coronavirus, despite being fully vaccinated, were almost twice as likely to have no symptoms at all, compared to the wider population.
The survey also found that the risk of breakthrough patients suffering from long-COVID, with symptoms lasting more than a month, were cut in half by full vaccination.
The age distribution of breakthrough cases is similar to non-vaccinated COVID patients. Three-quarters of the breakthrough cases in the US were 65 or older.
Is herd immunity achievable?
Herd immunity can be a confusing topic because it means different things in different circumstances.
At a general level, herd immunity occurs when a significant portion of a population becomes immune to an infectious disease, limiting further disease spread. Those who are not immune are indirectly protected because the ongoing transmission of the disease is small.
Currently, people who cannot be vaccinated, like children under 12, are best protected by insulating them by having everybody around them in the community vaccinated.
Herd immunity can also mean that at a certain vaccination level, the transmission of a virus is stopped because it effectively runs out of people to infect. That required vaccination rate among the population depends on the reproductive number of the virus, or how many people one infected person will on average transmit the virus to.
Measles is often given as an example because it has a reproductive number of 12 or higher, which requires more than 90% of the population to be immune as a result of either infection or vaccination.
Vaccination rates of more than 90% have led to few outbreaks of the disease in the US over the last decade until 2019 when hesitancy among parents to have their children vaccinated brought down immunisation rates.
While having a high vaccination rate is important to protect the most vulnerable and those who cannot be vaccinated, reaching herd immunity, that would stop the spread of the coronavirus entirely, may be difficult to achieve.

This is because of widespread vaccine hesitancy, the emergence of new more-contagious variants and the inability to vaccinate children at this stage. Breakthrough cases affecting the COVID-vaccinated are another factor.

Breakthrough cases for measles, for instance, are even rarer than for COVID, because the vaccines are more effective (97%) and those who are vaccinated rarely interact with those who are infected.
This is not the case with the widespread coronavirus and breakthrough infections are likely to continue. In practice, this means that COVID-19 is expected to become an endemic disease, much like influenza, that exhibits occasional or seasonal surges.
In this context, it is important to remember that vaccination is not the only form of prevention.
Hand hygiene, mask-wearing and social distancing also effectively lower the transmission of the virus and therefore behavioural changes will impact the required immunisation among the population to keep COVID-19 from spreading.
Related Videos








Thanks for an excellent review of the data and implications.
In my opinion this is an excellent article. The main message—-get vaccinated to protect yourself, your family and the community!
This is the first time that I have read an objective, scientific, statistical discussion of the risk to the island. Bravo!
GET VACCINATED!!
Nowhere in your article did anyone address the use of Monoclonal antibodies or Remdesivir (antivirals) before having to be put on ventilators. I mentioned these treatments in your article “11,000 new vaccines”. Please have all the necessary tools to treat this virus ahead of reopening. Thanks!
Excellent article. Thoroughly and assiduously researched.
Very Happy to hear they realize this is part of our world now and being vaccinated is a way to show our strength to survive. It is not going away .
Embrace it and fight back with being vaccinated.
So basically what I get from this article is that we are holding everyone hostage in order to prevent what could be very little who end up hospitalized or face death from the virus and that we are more than equipped to handle these cases. So why aren’t we reopening?
The charts you shown for Bermuda don’t tell the entire story because it doesn’t account for the 67% vaccination rate.
Unfortunately the chart doesn’t say if that’s 67% of the whole population or of the adults population.
Let’s assume it’s the adult population.
The population of Bermuda is 64,000. Let’s assume that 40,000 are adults and thus eligible for vaccination. Then 67% of 40,000 (27,000) are vaccinated and 13,000 unvaccinated.
5 of the fully vaccinated ended up in hospital. That’s 0.02%.
116 of the unvaccinated ended up in hospital. That’s 1%.
Please get vaccinated folks.
BRAVO CC! Well laid out, and honest.
The CIG needs to stop coddling the un-vaccinated and start figuring out how to manage the un-vaccinated who get sick who will rarely end up in the hospital. Stop holding the vaccinated hostage. With numbers this low don’t you think it’s about time to let the hospitals and Dr.’s do their job?
My guess is that at best they will open for tourism next summer when the initial volume of possible tourists will be at its lowest.
But I have one question. Will the CIG accept the U.S. CDC vaccination cards? Or will they forever cling to the CIG’s digital vaccination verification process? If they do they will only shoot themselves in the foot – again.
An excellent, well-researched, article by Mr. Klein and Mr. Whittaker. Congratulations to the Cayman Compass for finally researching all the relevant information concerning the morbidity and mortality rates of Covid-10, especially as it relates to vaccination rate.
My only question is: Why did it take so long? It’s too bad that this wasn’t published 2 weeks ago; perhaps it might have convinced the Premier to hold off reversing his plan to open the island to tourism again. Then again, since the government has always said it wants to “follow the science,” perhaps they might consider putting plan back in motion again.
Excellent article. Well thought out and enlightening. Hope this encourages those on the fence to get vaccinated. There is no doubt that the vaccine protects the vaccinated from serious disease and death. I sincerely hope this is not behind the paywall. Because it would be a shame if it was only viewed by choir.
Excellent article. Articulate, clear and fair. Also thank you for reminding us that the whole purpose of closing our borders in the first place was to PREVENT OUR HOSPITALS BEING OVERRUN! Well we certainly did that with bells on! Now we need to get on with opening up – using the science, the statistics and the vaccination. This is a virus and it is here to stay!
Excellent article with good data. I will say that the only thing missing is data to help ameliorate the fears with regard to the risk to children under 12 years old.
The chances of unvaccinated children under 12 of dying from Covid is 1 in 500,000. In perspective children are:
Equally likely to die in a fire
3x more likely to drown
7x more likely to die of cancer
9x more likely to die in car accident
36x more likely to die from injury, in general
Moreover, vaccinated people 50 years or less have the share similar probabilities as described above.
So at this point, if we do open up fully, our children are at the same benign risk as we have dealt with in their day-to-day lives prior to the emergence of the virus. Given this, I think we can all take a deep breath of relief and move on with our lives.
https://researchaddict.com/covid-children-risk/
“when and if the virus enters our community”
“If”? How poorly informed can government be.
The proof was in the pudding. The local infections materialised and the government panicked.